Healthcare in America vs Socialized Medicine Today
1. What We Have Now (U.S. Model)
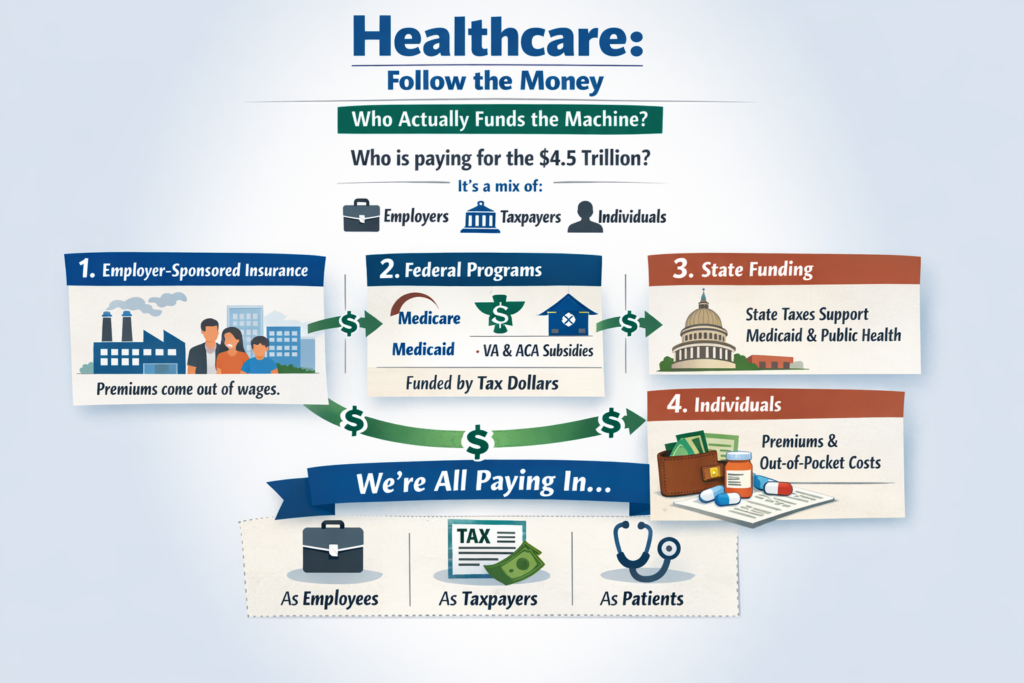
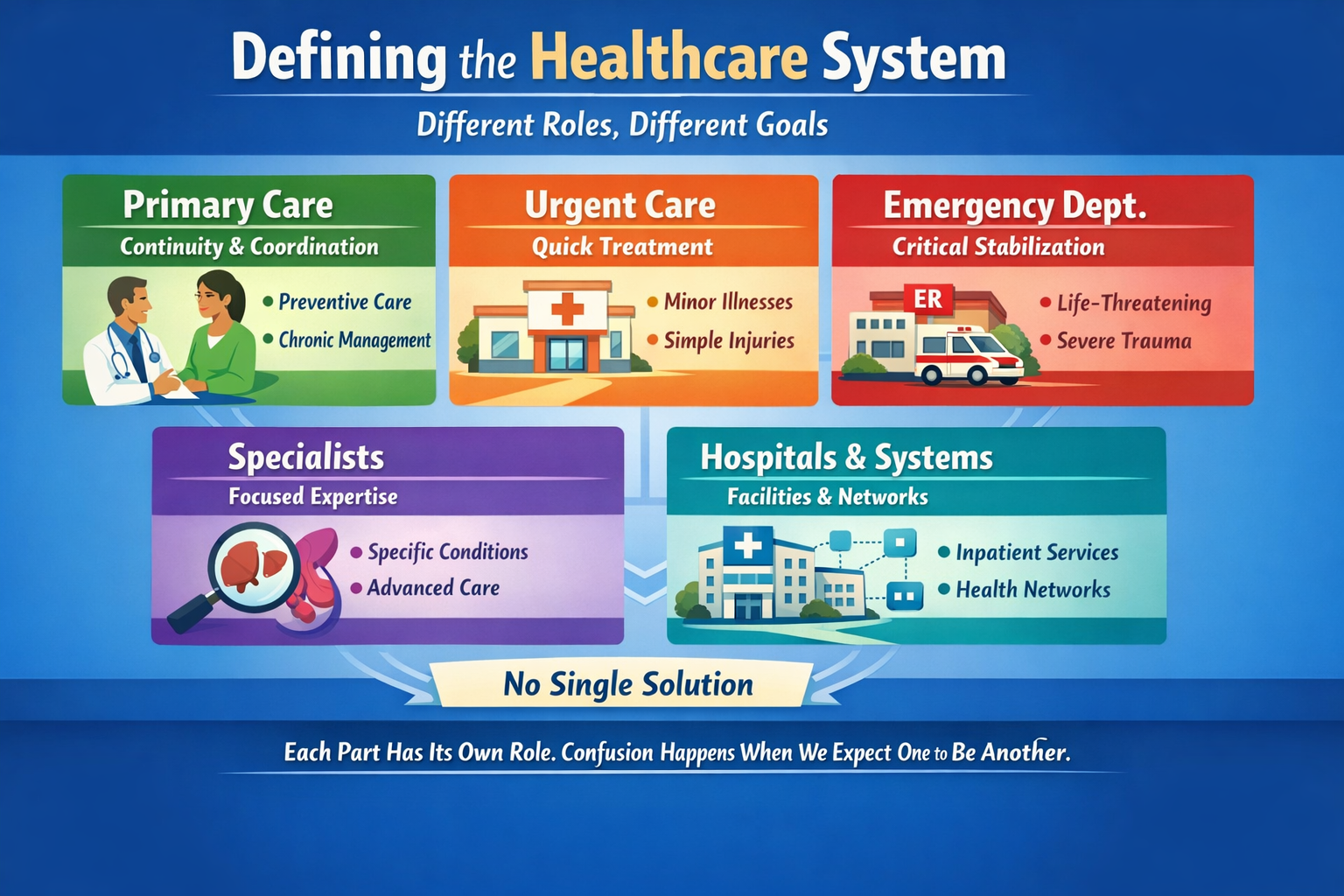
The U.S. system is a hybrid, multi-payer system:
-
Private insurance (employer-based and individual market)
-
Public insurance:
-
Medicare
-
Medicaid
-
TRICARE
-
Veterans Health Administration
-
-
Private hospitals (mostly nonprofit, some for-profit)
-
Private physician practices (increasingly consolidated)
Important reality:
Roughly half or more of U.S. healthcare spending already flows through government programs. We are not a pure market system. We are a complex blend.
2. What “Socialized Medicine” Actually Means
People often use “socialized” loosely. There are actually three different models internationally:
A. Fully Socialized (Government Owns & Employs)
Example: National Health Service in the UK
-
Government owns hospitals
-
Doctors are government employees
-
Government sets budgets directly
-
Care funded through taxes
That’s true “socialized medicine.”
B. Single-Payer (Government Pays, Private Providers Deliver)
Example: Medicare (Canada’s system)
-
Private hospitals & doctors
-
Government is the main insurer
-
One public payment system
-
Funded via taxes
This is not government-run hospitals — it’s government-run insurance.
C. Multi-Payer Regulated System
Example: Statutory Health Insurance
-
Private and nonprofit insurers
-
Strict national rules
-
Price controls
-
Universal coverage mandate
3. So How Different Are We?
Structurally:
-
We already have heavy government financing.
-
We already regulate pricing in public programs.
-
We already operate large government-run care systems (VA hospitals).
-
We already subsidize private insurance through tax exclusions.
What we don’t have:
-
A unified payment structure
-
National price controls across the board
-
Universal automatic coverage
-
Simplified billing
The biggest structural difference isn’t just “who pays.”
It’s:
-
Fragmentation
-
Administrative layering
-
Pricing freedom in private markets
-
Employment-tied insurance
4. Where the Real Divide Is
The debate isn’t simply:
Private vs Socialized.
It’s about:
-
Who controls pricing?
-
How risk is pooled?
-
How incentives are aligned?
-
How much administrative complexity is tolerated?
Even a “socialized” system still rations care — just differently (wait times vs cost-sharing).
Even our current system has price controls — just unevenly applied.
5. If the U.S. “Moved Toward Socialized” — What Would Actually Change?
Not necessarily hospital ownership.
More likely changes would include:
-
Centralized bargaining power
-
Uniform reimbursement rates
-
Elimination of employer-based insurance
-
Tax-based funding instead of premium-based funding
-
Dramatically reduced administrative overhead
-
Reduced insurer role
The money flow changes.
The power centers shift.
Administrative structure simplifies.
But doctors would still practice medicine.
Hospitals would still exist.
Care would still be rationed — just through different mechanisms.
6. The Quiet Truth
We are already halfway between models.
The U.S. system is not a free market.
It is not socialized.
It is a layered hybrid with competing incentives.
The question isn’t:
“Would we become socialized?”
The real question is:
“How centralized do we want payment and pricing authority to be?”
That’s a structural debate — not just a funding debate.
To go deeper, we have to explore:
-
What would actually happen to costs?
-
What happens to innovation?
-
What happens to wait times?
-
Or what a realistic transition would look like?
The real questions aren’t ideological. They’re mechanical:




































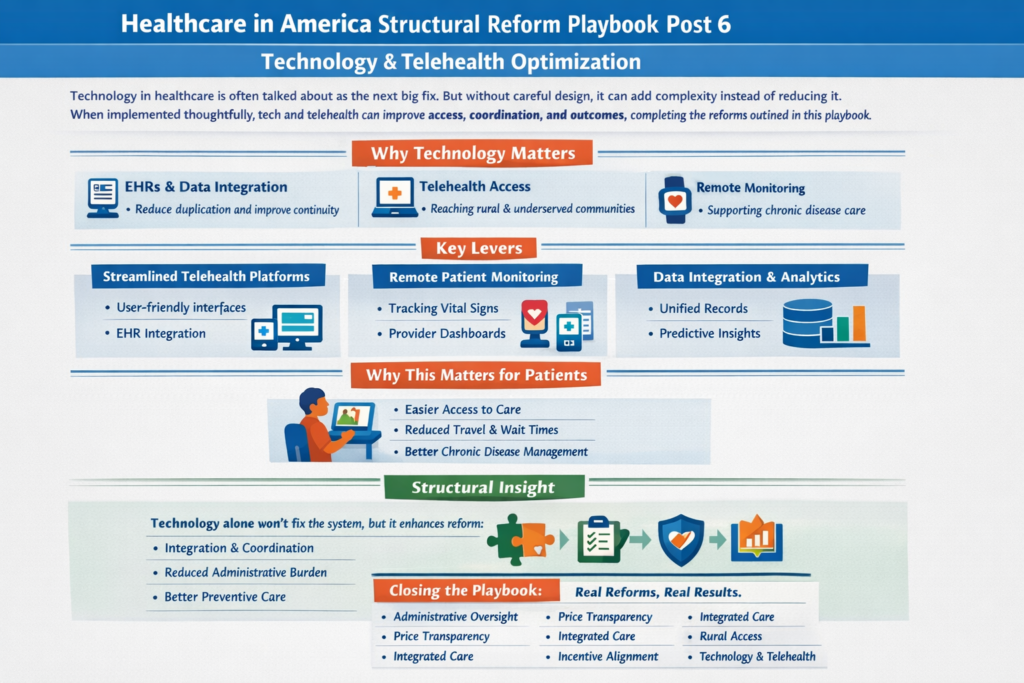









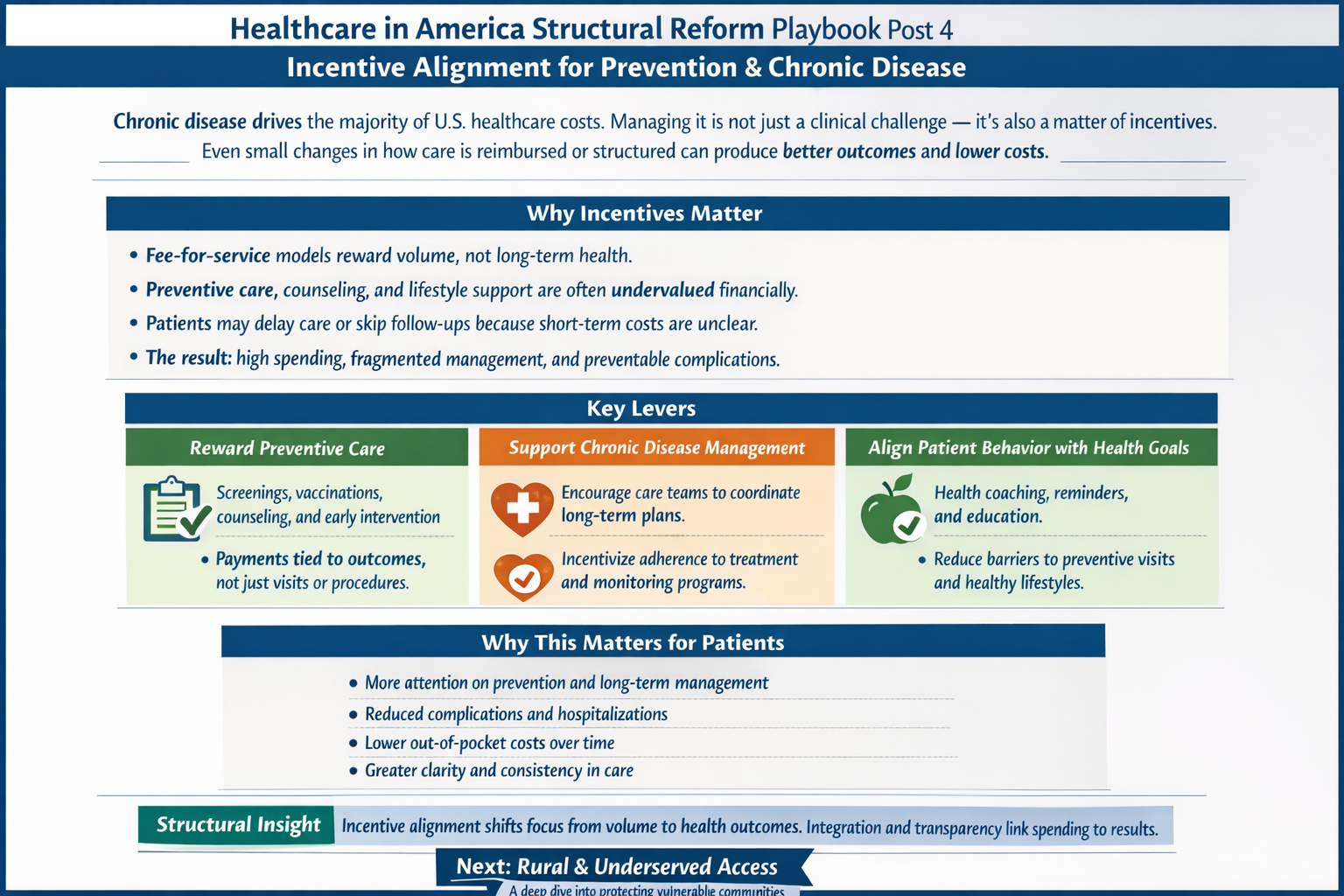

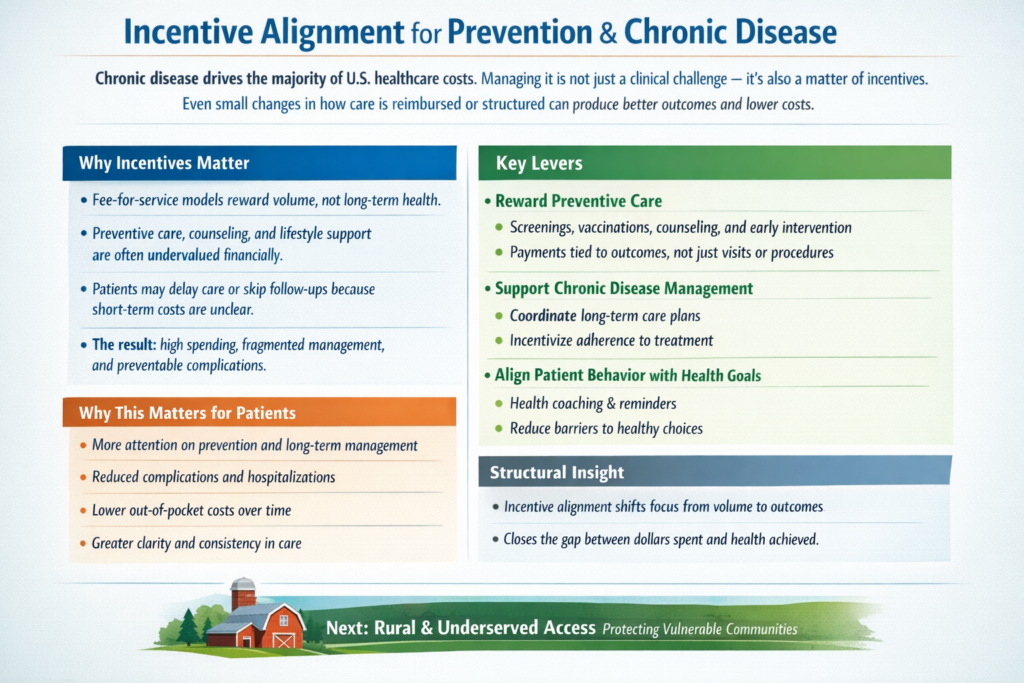






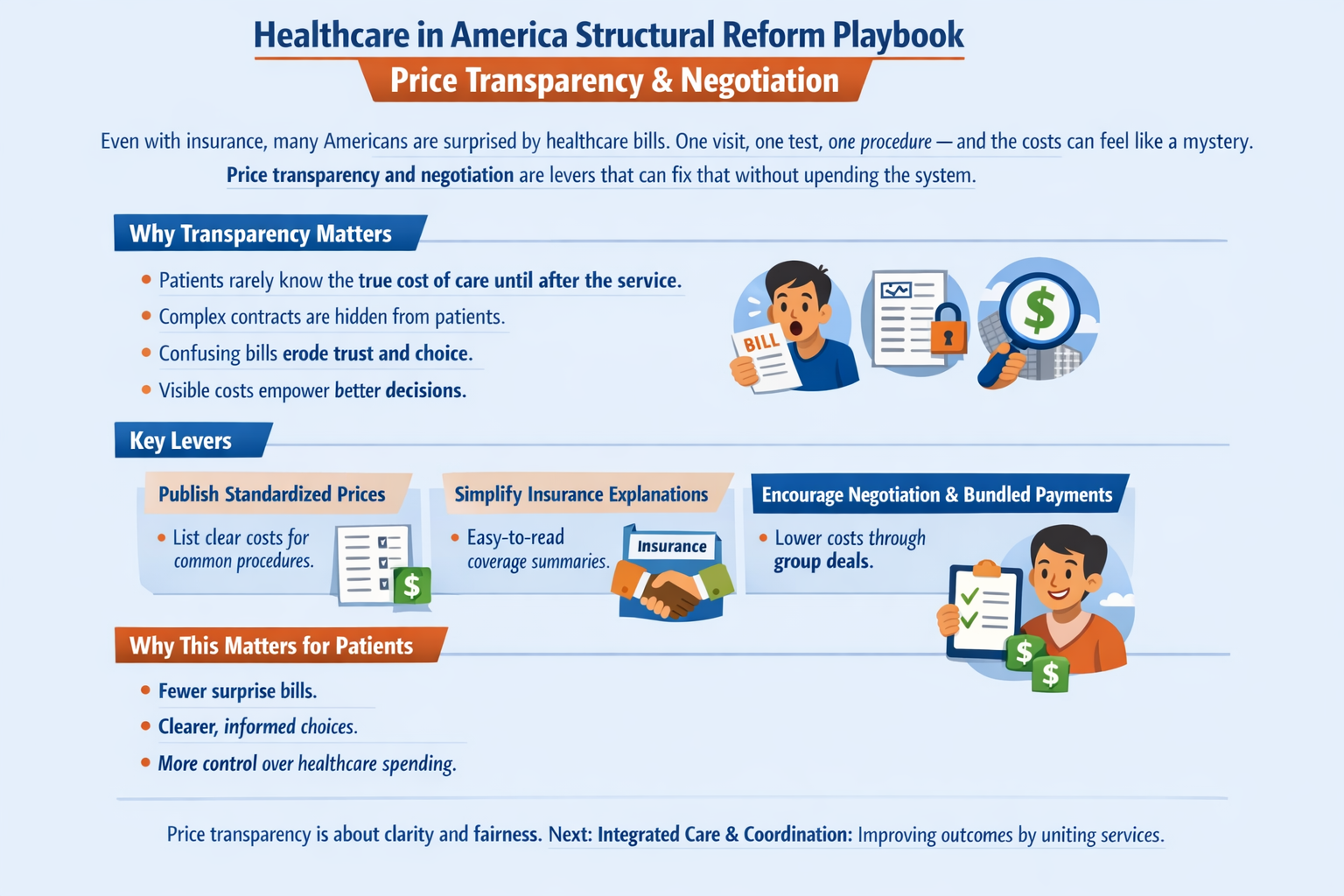







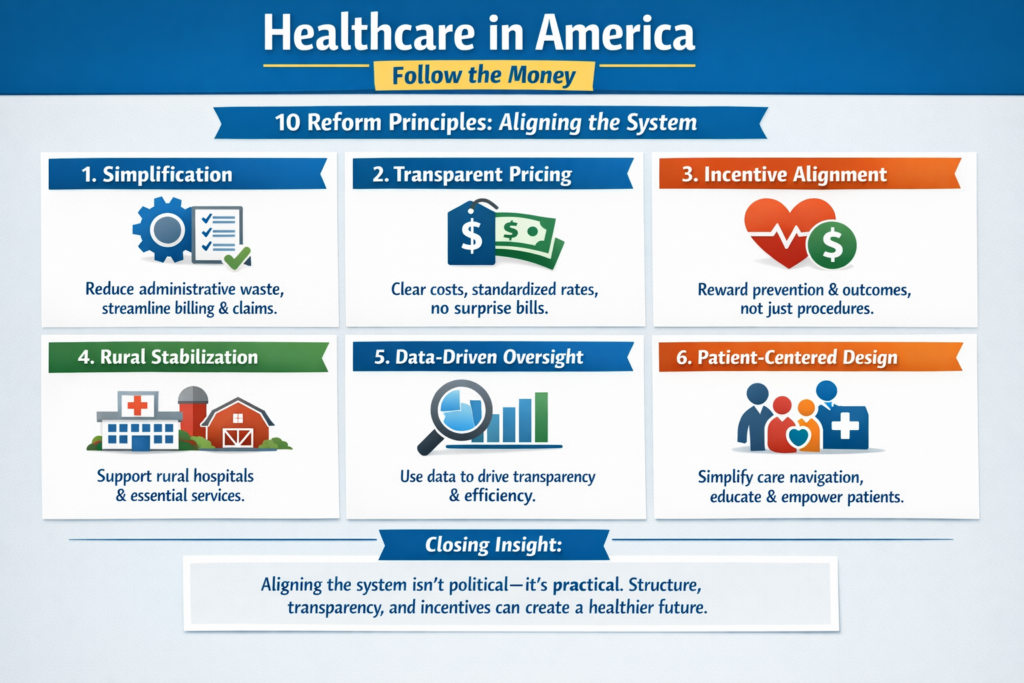


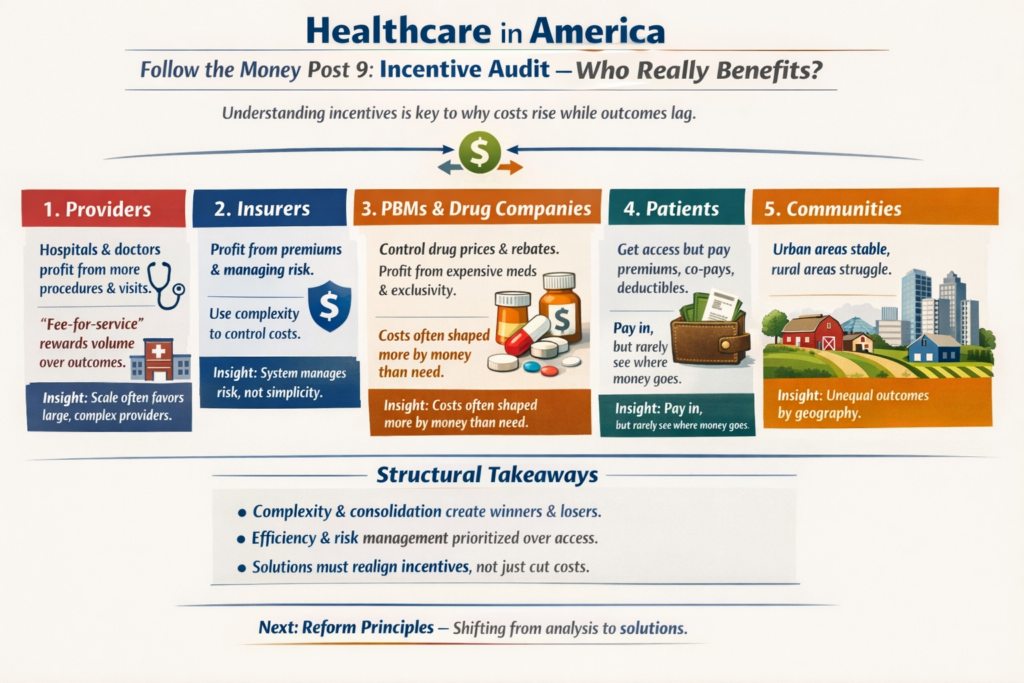
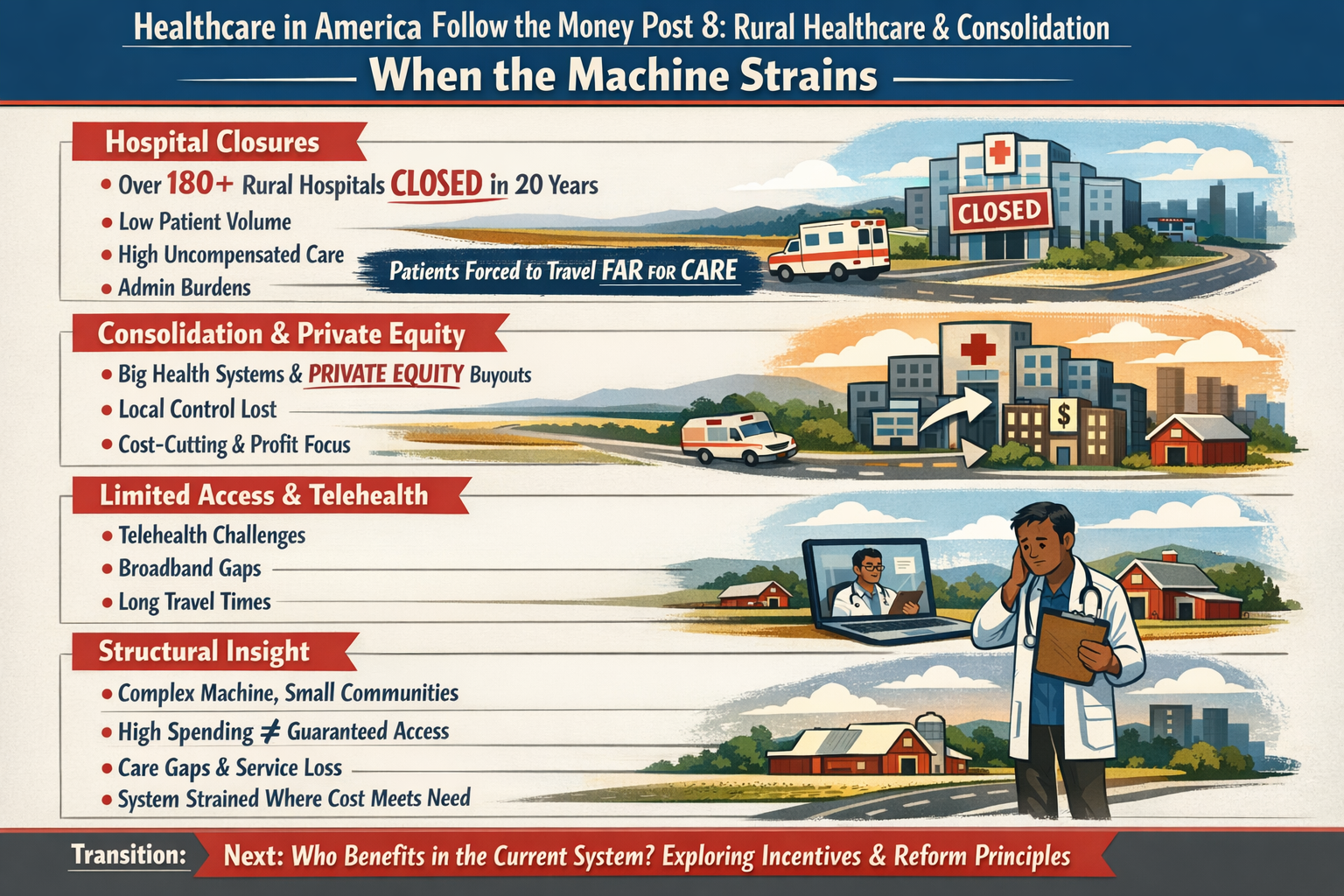


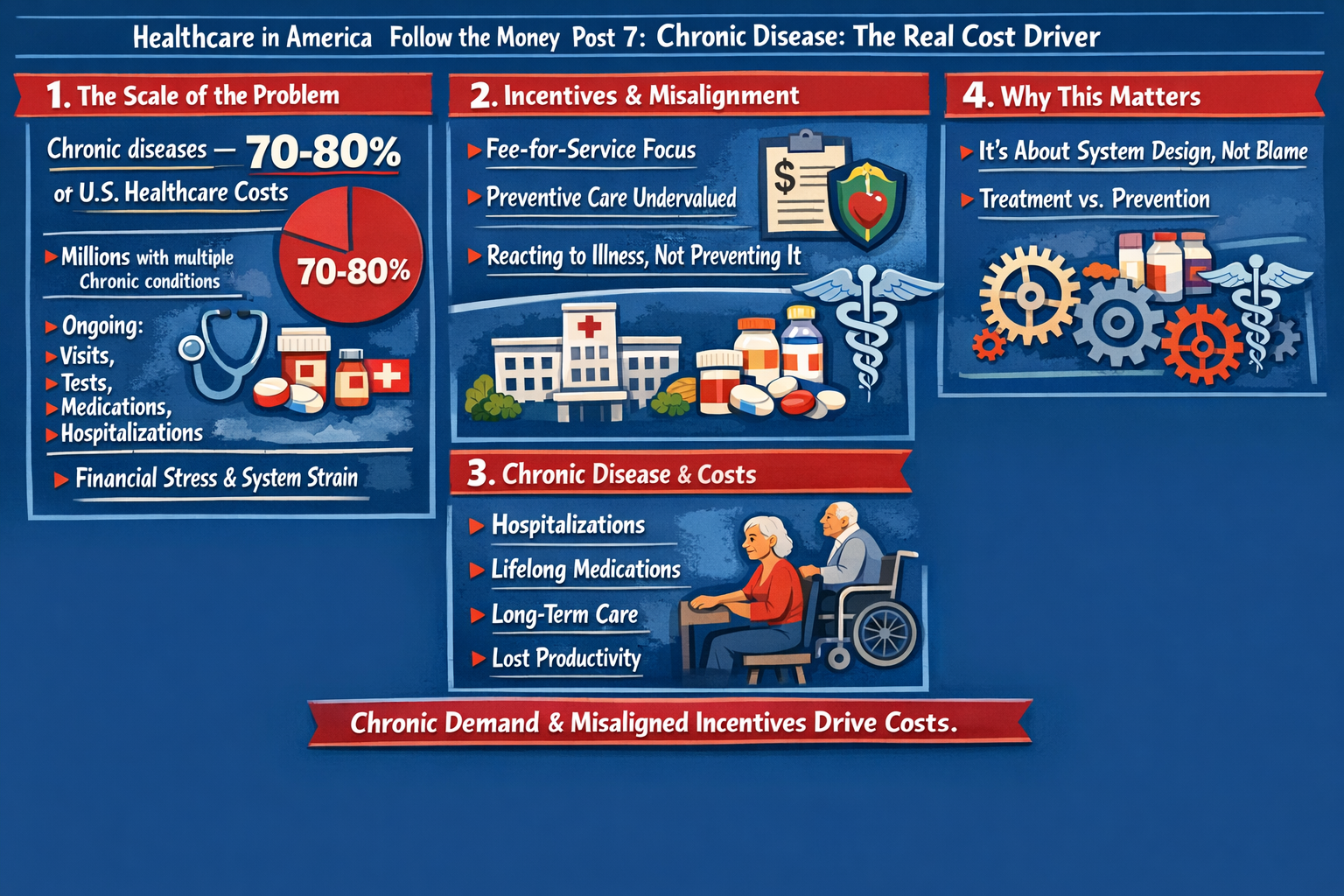





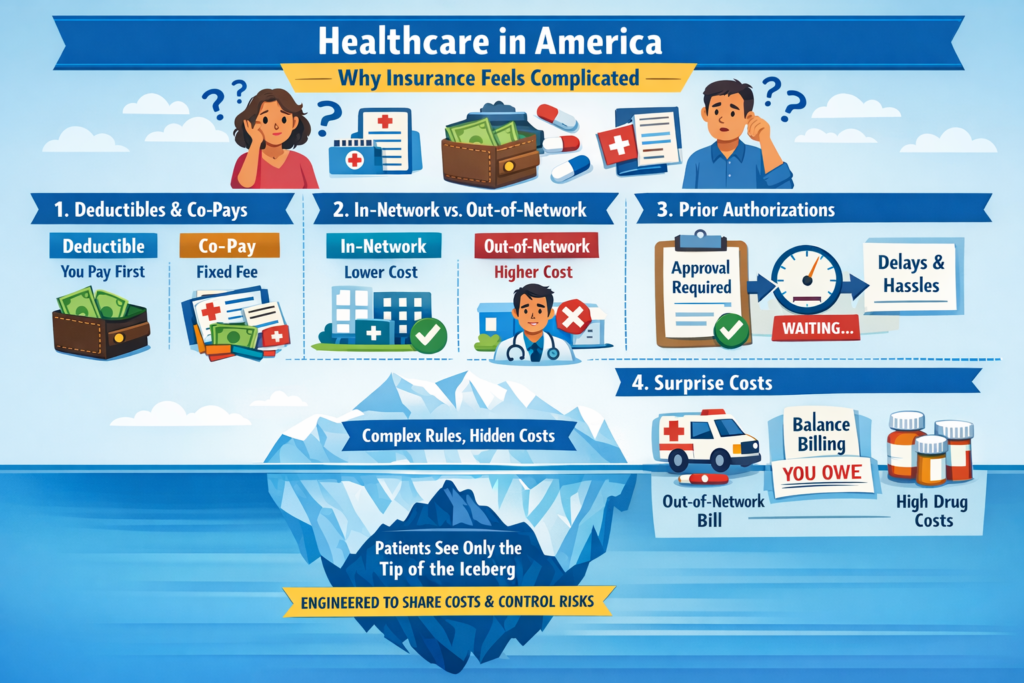


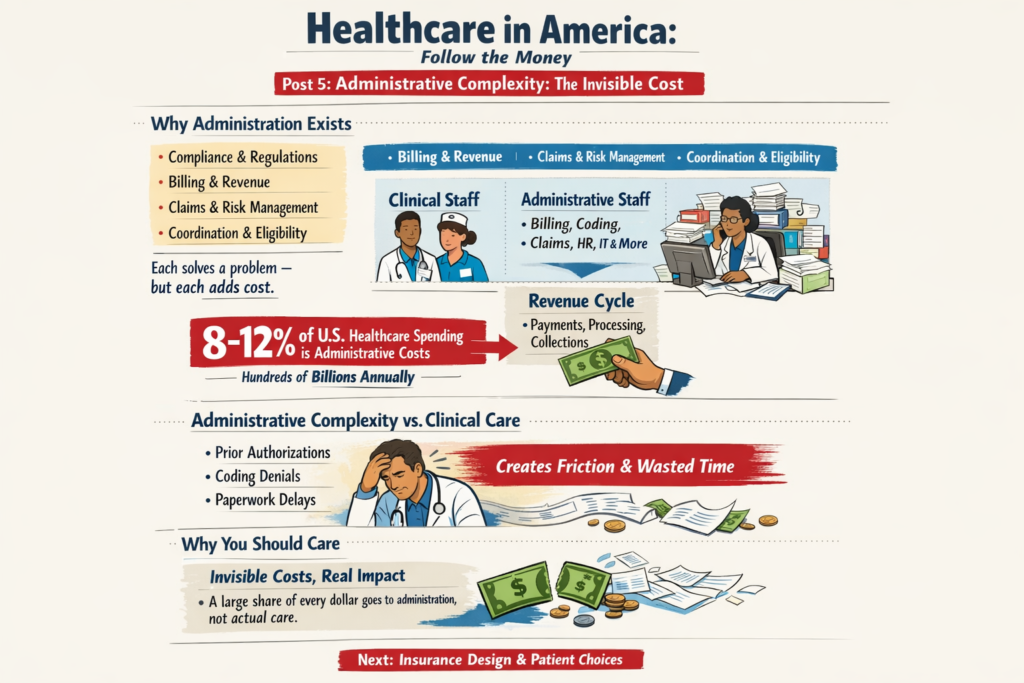
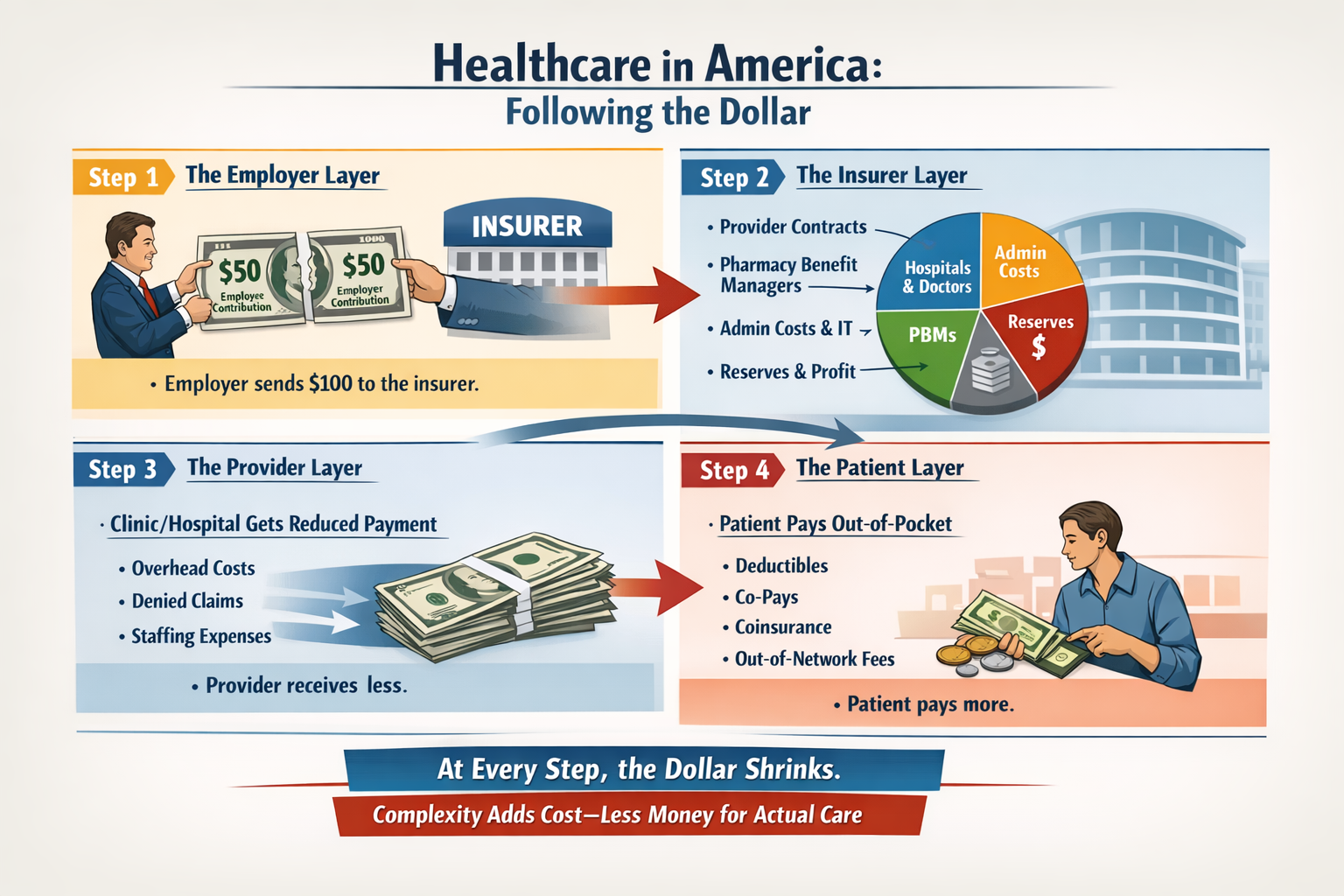

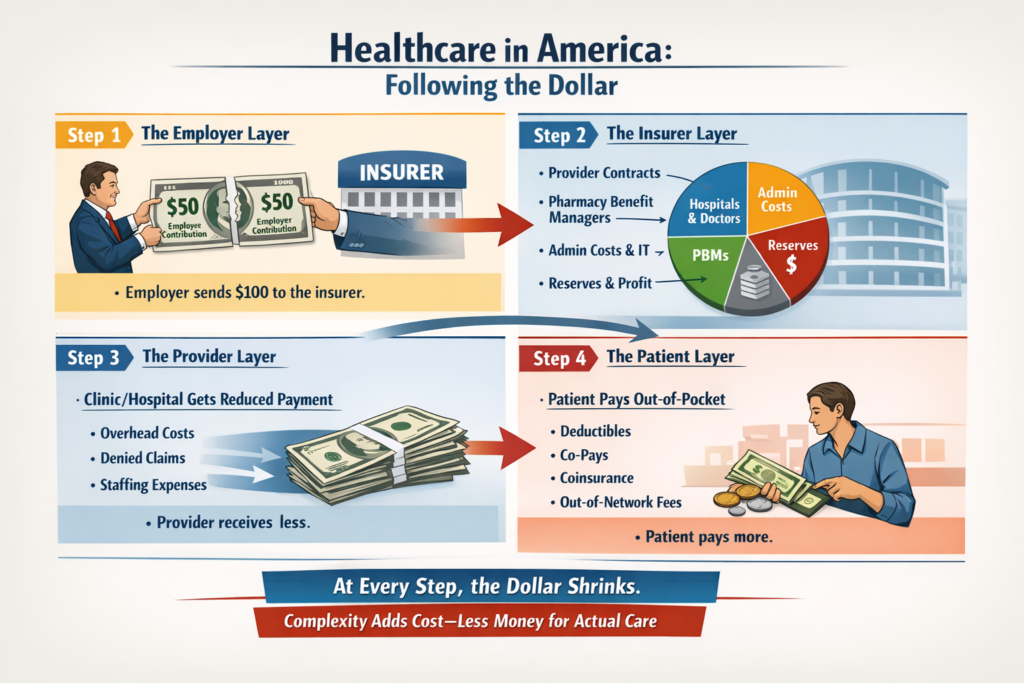
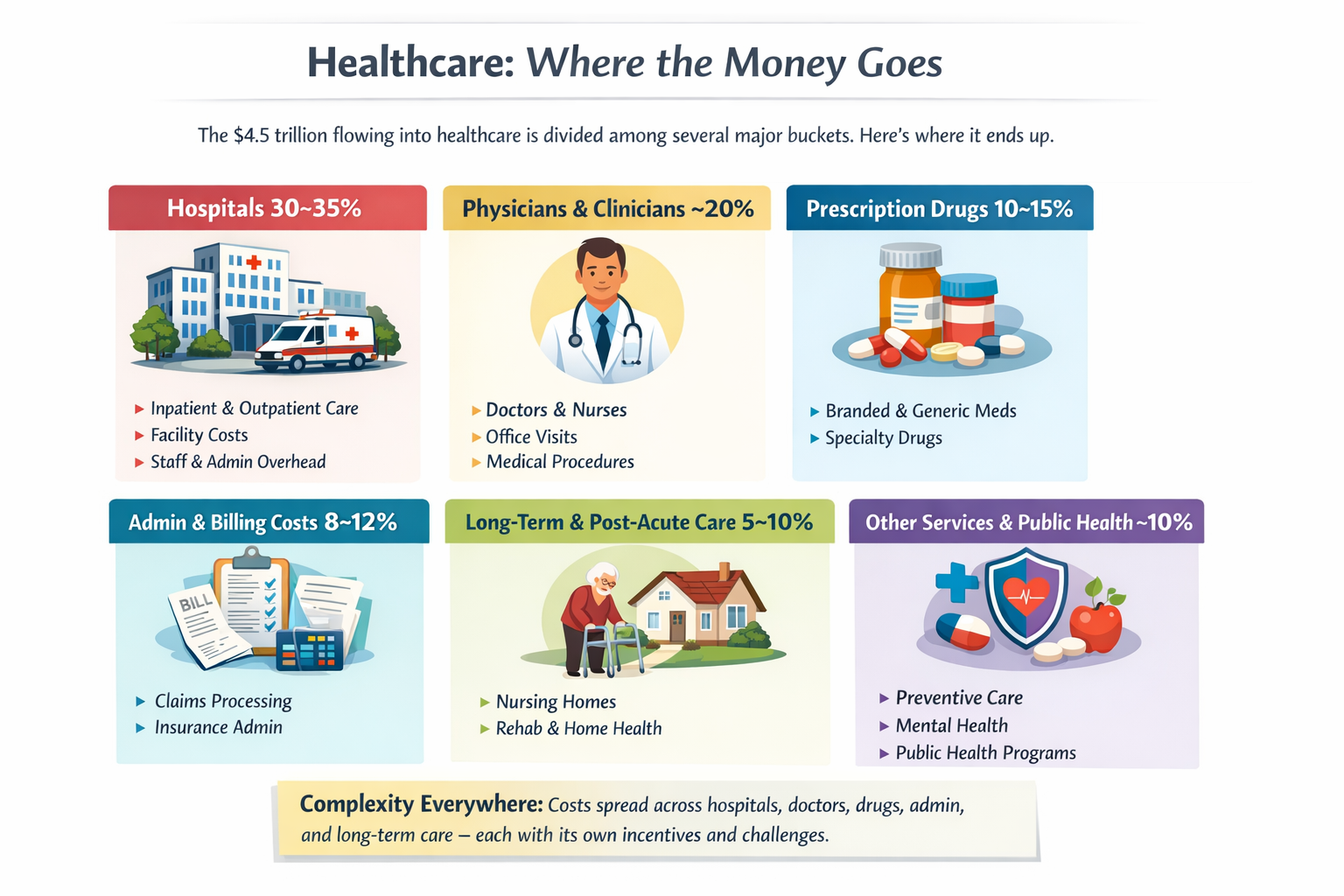
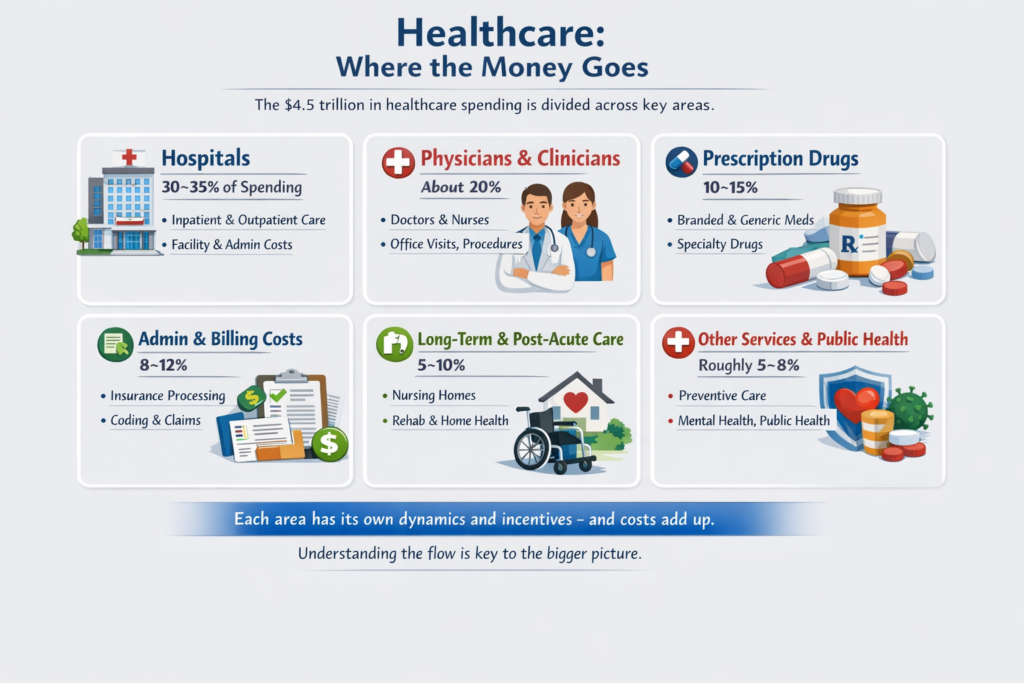







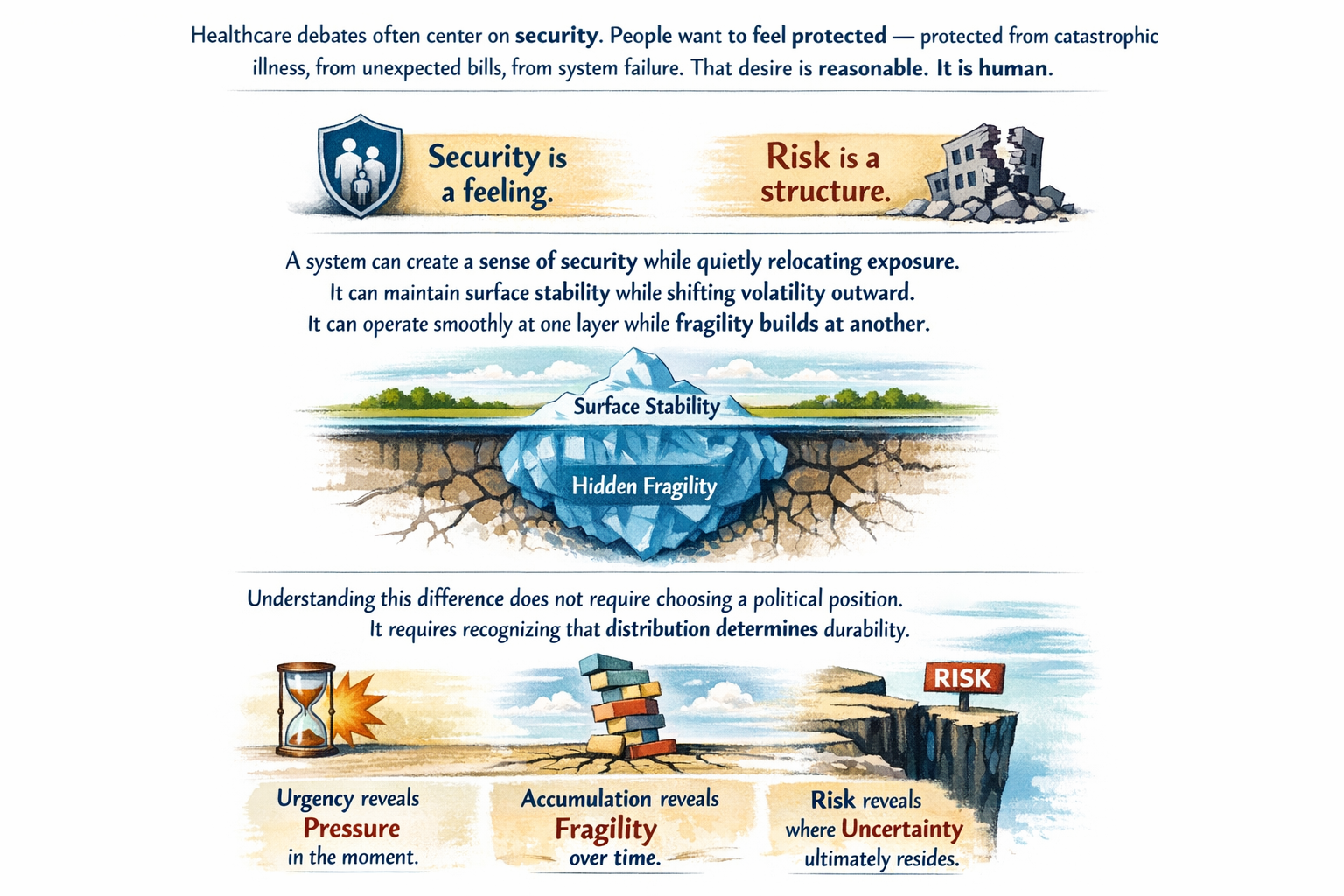






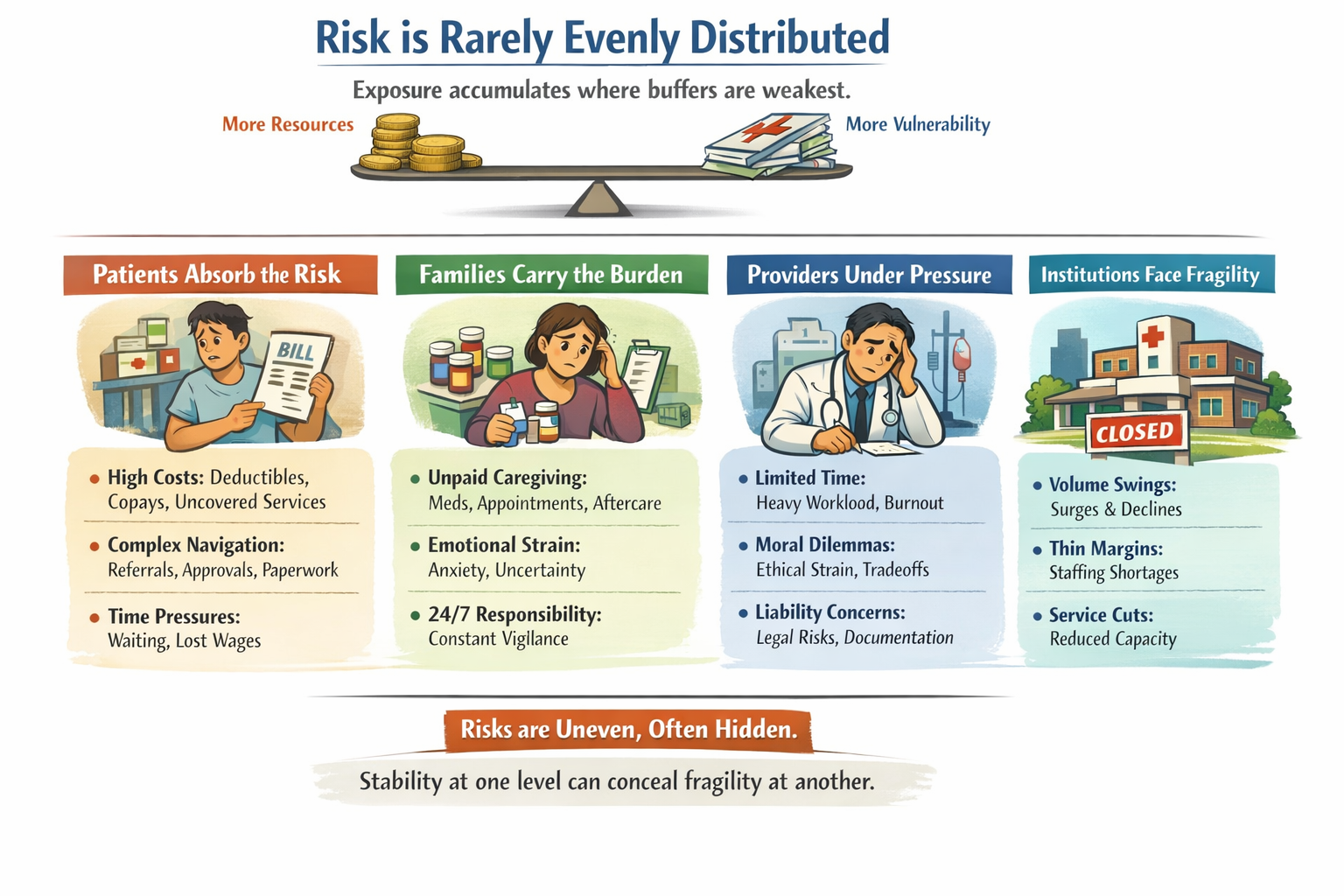












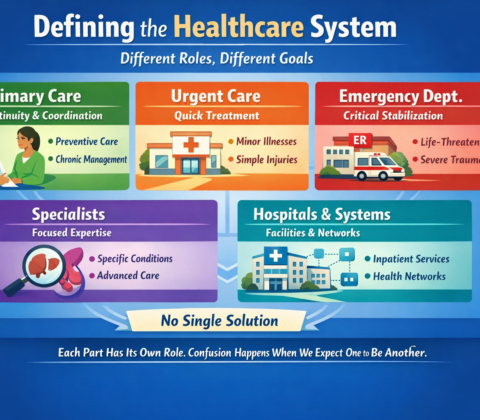











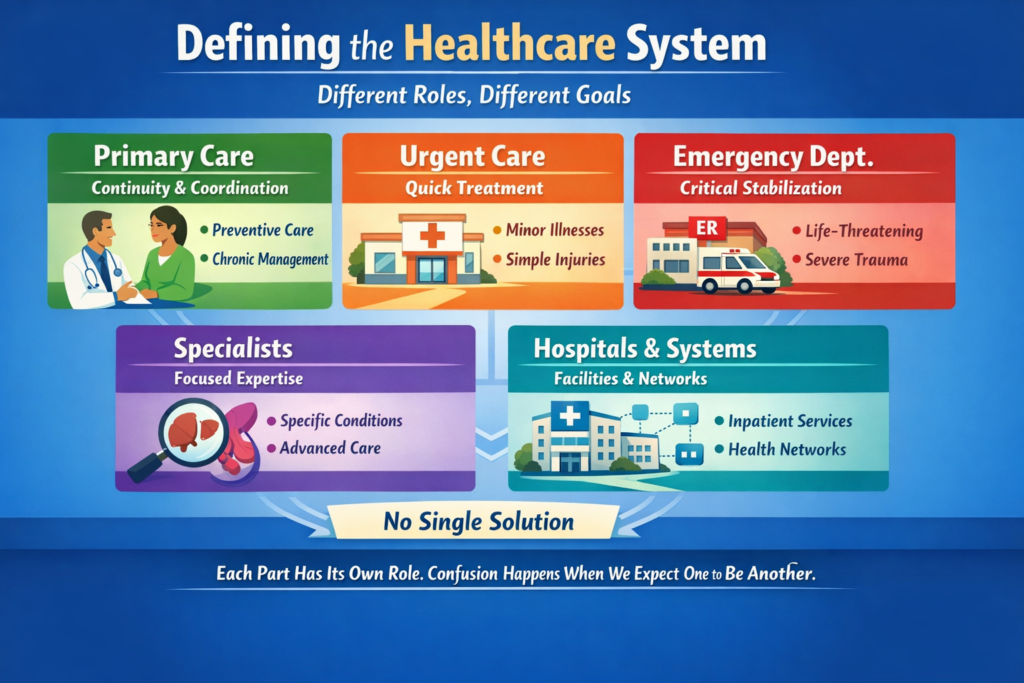
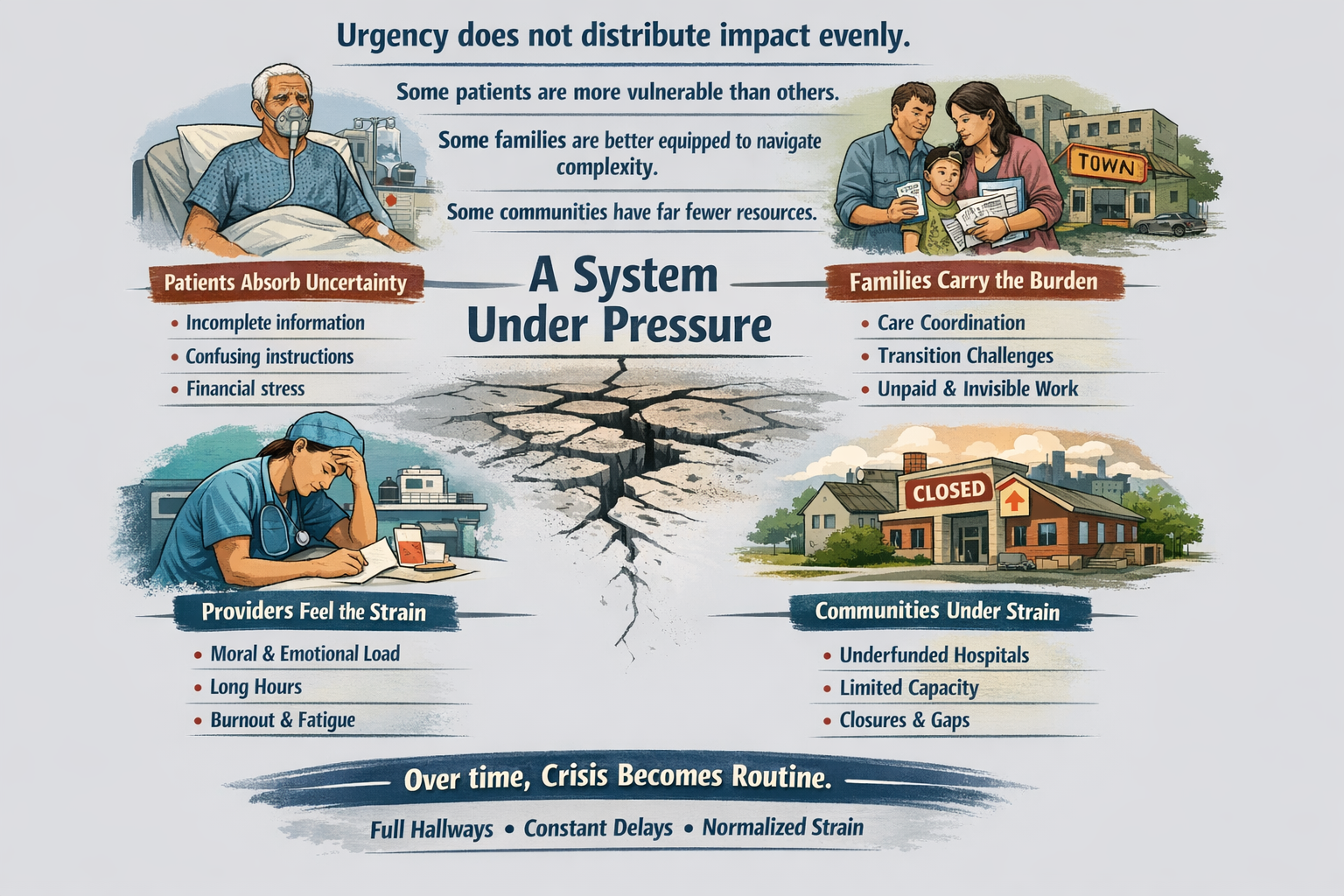
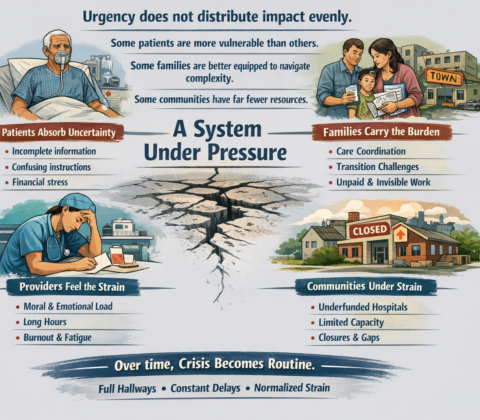


























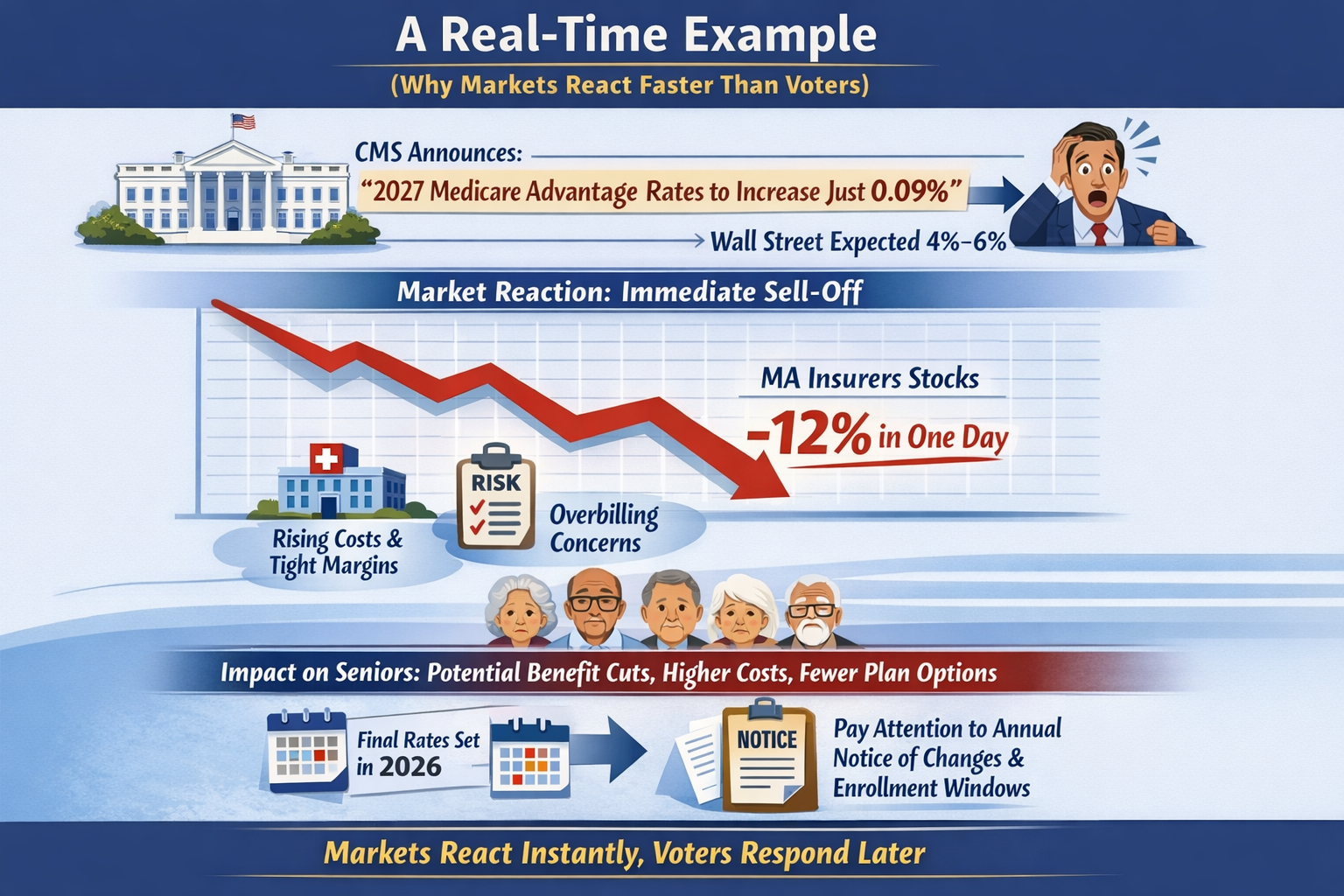
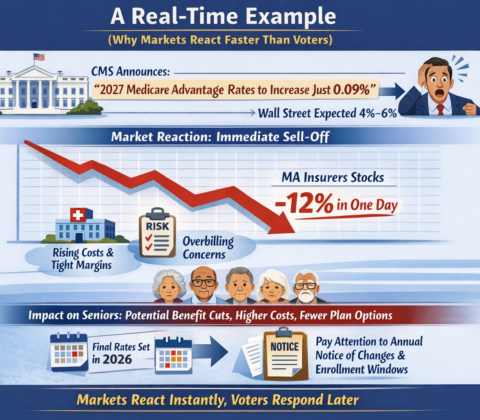

























































The Ripple Effect, The Cost of Donny the Toddler’s Revenge
We are in a strange environment where nothing feels as it was.
Because it isn’t as it was.
I have contracted in companies where the boss was a hands-on micromanager and every failure was blamed on whoever was closest. Never the real culprit. Never the micromanaging boss. It was never their fault.
Sound familiar?
When decisions are made with a sense of satisfaction, a score settled, a grievance answered, to the person making them it feels like justice.
The action itself can seem small. A policy change. A funding cut. A shift in priorities framed as strength or loyalty. Something done not just because it is believed to be right, but because it answers a need to get even. To punish an enemy.
A stone dropped into still water.
At first nothing dramatic happens. Just a small disturbance. A ripple that feels contained, manageable, even insignificant.
But ripples don’t stay where they begin.
They move outward, quietly, steadily, touching places far removed from the original decision. People who were never part of the argument. Communities that had no voice in the conflict. Families who don’t follow the headlines closely but live with the outcomes.
A clinic closes earlier than it should.
A farmer faces one more season with less support.
A family sits at a table trying to make numbers work that no longer do.
None of them were in the room when the decision was made.
None of them were the target.
But they feel the result all the same.
This is the danger of governance driven by grievance rather than responsibility. The intent may be narrow, focused on winning, punishing, proving a point, but the consequences are not.
They spread.
Leadership isn’t measured by the force of the initial action or the satisfaction it brings in the moment. It’s measured by how far those ripples travel and who they reach when they arrive.
Our government is being run by a micromanager governing out of grievance, without care or foresight for the damage the ripples of his decisions are creating.
Sometimes a ripple becomes a tsunami.
Who is going to clean up the carnage?
Share this:
Like this: