Healthcare in America Structural Reform Playbook Post 4 Incentive Alignment for Prevention & Chronic Disease

Healthcare in America Structural Reform Playbook Post 4 Incentive Alignment for Prevention & Chronic Disease
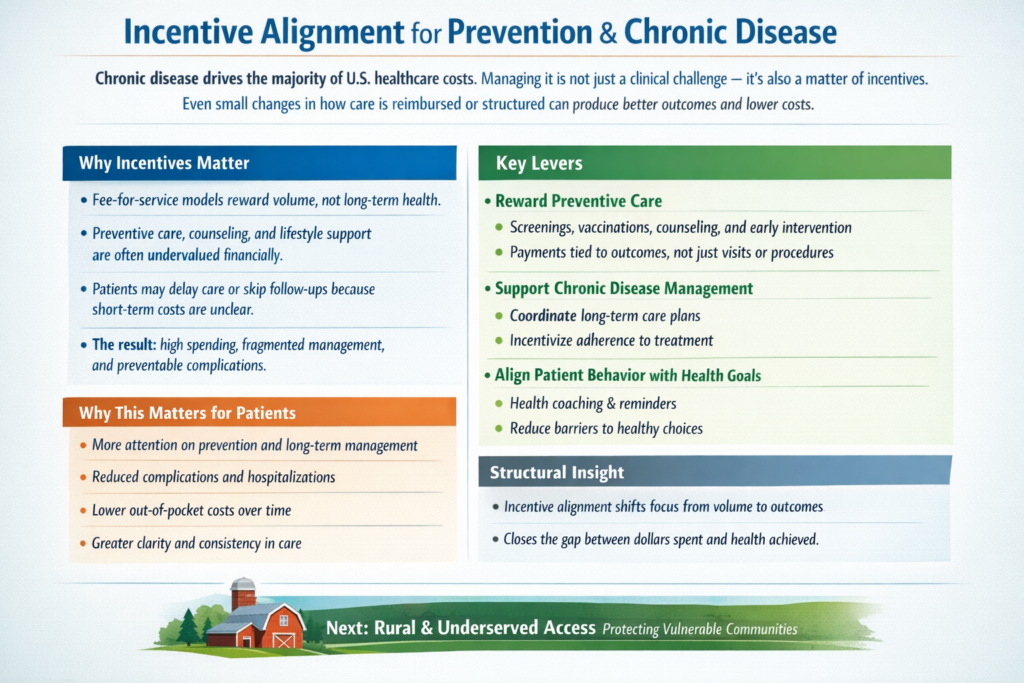
Chronic disease drives the majority of U.S. healthcare costs. Managing it is not just a clinical challenge — it’s also a matter of incentives. Even small changes in how care is reimbursed or structured can produce better outcomes and lower costs.
Why Incentives Matter
-
Fee-for-service models reward volume, not long-term health.
-
Preventive care, counseling, and lifestyle support are often undervalued financially.
-
Patients may delay care or skip follow-ups because short-term costs are unclear.
The result: high spending, fragmented management, and preventable complications.
Key Levers
-
Reward Preventive Care
-
Screenings, vaccinations, counseling, and early intervention
-
Payments tied to outcomes, not just visits or procedures
-
-
Support Chronic Disease Management
-
Encourage care teams to coordinate long-term plans
-
Incentivize adherence to treatment and monitoring programs
-
-
Align Patient Behavior with Health Goals
-
Use tools like health coaching, reminders, and education
-
Reduce barriers to preventive visits and healthy lifestyle adoption
-
Why This Matters for Patients
-
More attention on prevention and long-term management
-
Reduced complications and hospitalizations
-
Lower out-of-pocket costs over time
-
Greater clarity and consistency in care
Structural Insight
-
Incentive alignment does not require a system overhaul.
-
Shifting focus from procedure volume to health outcomes produces measurable improvements.
-
When paired with integration and transparency, it closes the loop between dollars spent and health achieved.
Transition
Next in the playbook: Rural & Underserved Access, a deep dive showing how structural levers can protect vulnerable communities and preserve essential services.